Why Milestones Matter for Safe Return to Activity
Rehab milestones provide objective checkpoints—pain‑free ROM, 80‑90% strength symmetry, functional tests, and psychological readiness—ensuring tissue healing before higher‑impact loads. Chiropractic care accelerates these phases by restoring joint mechanics, reducing pain, and enhancing neuromuscular control through adjustments and soft‑tissue work, while integrating progressive strength and balance exercises. In Glenwood Springs’ high‑altitude, outdoor‑focused environment, clinicians tailor run‑walk intervals, cross‑training, and seasonal conditioning to match local terrain and climate, promoting safe, individualized return to activity.
Early Warning Signs and Healing Phases
Early Warning Signs & Healing Phases
| Warning Sign | Description | Possible Serious Injury |
|---|---|---|
| Persistent pain/swelling > few days | Deep tissue or bone damage not resolving | Fracture, ligament tear, internal bleeding |
| Severe headache, dizziness, confusion, LOC | Concussion or internal head trauma | Traumatic brain injury, intracranial bleed |
| Sudden loss of mobility, numbness, tingling, weakness | Nerve injury or spinal cord involvement | Radiculopathy, spinal fracture |
| Large bruised abdomen/chest with pain | Internal bleeding or organ injury | Splenic laceration, rib fracture, pulmonary contusion |
| Delayed symptoms that worsen (pain, fatigue, swelling) | Delayed but serious pathology | Sub‑dural hematoma, compartment syndrome |
| Healing Phase | Approx. Duration | Key Features | Chiropractic Support |
|---|---|---|---|
| Hemostasis | Minutes–Hours | Platelet clot formation, bleeding stop | Gentle positioning, bleeding control advice |
| Inflammatory | 0‑3 days | Swelling, redness, warmth, debris clearance | Soft‑tissue work, anti‑inflammatory modalities |
| Proliferation | 3‑21 days | Granulation tissue, collagen deposition, re‑epithelialization | Adjustments to improve alignment, controlled loading |
| Remodeling (Maturation) | 3 weeks‑months | Collagen re‑organization, scar contraction, functional restoration | Ongoing adjustments, therapeutic exercise, nutrition guidance |
 When patients present after a motor‑vehicle collision, clinicians must quickly identify red‑flag findings that suggest a serious injury. Five key warning signs are: (1) persistent pain or swelling that fails to improve within a few days, indicating possible deep tissue or bone damage; (2) severe headache, dizziness, confusion, or loss of consciousness, which raise concern for concussion or internal head trauma; (3) sudden loss of mobility, numbness, tingling, or weakness in an extremity, suggesting nerve injury or spinal cord involvement; (4) large, visibly bruised areas on the abdomen or chest accompanied by abdominal or shoulder pain, pointing to internal bleeding or organ injury; and (5) symptoms that emerge hours or days later and progressively worsen, such as delayed pain, fatigue, or swelling, which may signal a delayed but serious problem.
When patients present after a motor‑vehicle collision, clinicians must quickly identify red‑flag findings that suggest a serious injury. Five key warning signs are: (1) persistent pain or swelling that fails to improve within a few days, indicating possible deep tissue or bone damage; (2) severe headache, dizziness, confusion, or loss of consciousness, which raise concern for concussion or internal head trauma; (3) sudden loss of mobility, numbness, tingling, or weakness in an extremity, suggesting nerve injury or spinal cord involvement; (4) large, visibly bruised areas on the abdomen or chest accompanied by abdominal or shoulder pain, pointing to internal bleeding or organ injury; and (5) symptoms that emerge hours or days later and progressively worsen, such as delayed pain, fatigue, or swelling, which may signal a delayed but serious problem.
Post‑surgical wound healing follows four overlapping phases. First, hemostasis rapidly forms a platelet clot to stop bleeding. Second, the inflammatory phase brings immune cells to clear debris, producing swelling, redness, and warmth. Third, proliferation builds new tissue—granulation tissue, fibroblast‑derived collagen, and re‑epithelialization close the wound. Finally, remodeling (or maturation) reorganizes collagen, contracts the scar, and restores functional integrity over weeks to months. Throughout these stages, evidence‑based chiropractic care—gentle adjustments, soft‑tissue work, and targeted therapeutic exercises—can support joint mechanics, reduce pain, and promote optimal tissue alignment, while complementary modalities such as nutrition optimization and low‑impact cross‑training help patients stay active without jeopardizing healing.
Exercise Frequency and Athlete Fundamentals
Exercise Frequency & Athlete Fundamentals
| Activity Type | Recommended Frequency | Rest Interval | Key Notes |
|---|---|---|---|
| Mobility / Flexibility / Movement‑Control Drills | 5‑7 days/week (daily) | None required | Keeps joints supple, reinforces neuromuscular patterns |
| Strength / Hypertrophy (early phase) | 2‑5 sessions/week | ≥48 h between sessions | Gentle loads early, progress to 2‑3 structured sessions later |
| Early‑phase gentle exercises | 3‑5 times/day | None (if pain‑free) | Focus on low‑load, pain‑free range of motion |
| Later‑phase structured strength | 2‑3 sessions/week | ≥48 h between sessions | Higher load, monitor for soreness |
| Consistency Pillars | Commitment, Consistency, Communication | — | Adherence prevents delayed collagen remodeling and re‑injury risk |
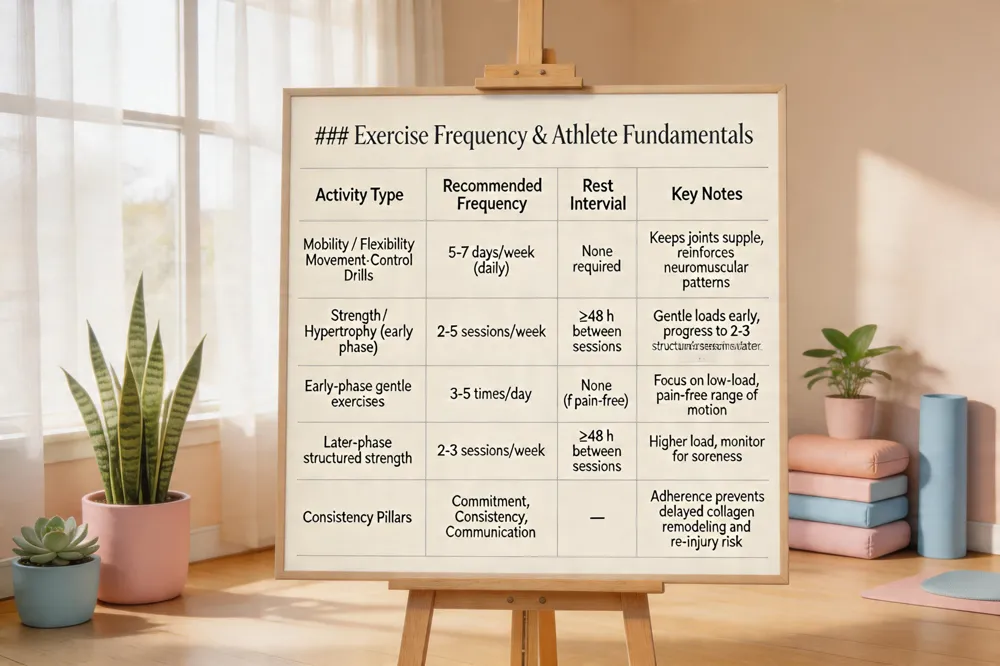 A well‑designed rehabilitation program balances tissue healing with functional conditioning. Evidence from chiropractic and sports‑medicine guidelines shows that mobility, flexibility, and movement‑control drills should be performed almost daily—5 to 7 days per week—to keep joints supple and reinforce proper neuromuscular patterns. Strength and hypertrophy work, which places greater stress on healing tissues, is best limited to 2 to 5 sessions per week with at least 48 hours of rest between sessions; early‑phase protocols may call for gentle exercises 3‑5 times daily, while later phases transition to 2‑3 structured sessions weekly. Consistency is essential—skipping days can delay collagen remodeling, prolong inflammation, and increase re‑injury risk.
A well‑designed rehabilitation program balances tissue healing with functional conditioning. Evidence from chiropractic and sports‑medicine guidelines shows that mobility, flexibility, and movement‑control drills should be performed almost daily—5 to 7 days per week—to keep joints supple and reinforce proper neuromuscular patterns. Strength and hypertrophy work, which places greater stress on healing tissues, is best limited to 2 to 5 sessions per week with at least 48 hours of rest between sessions; early‑phase protocols may call for gentle exercises 3‑5 times daily, while later phases transition to 2‑3 structured sessions weekly. Consistency is essential—skipping days can delay collagen remodeling, prolong inflammation, and increase re‑injury risk.
Athletes should also anchor their rehab around the three “C’s”: Commitment, Consistency, and Communication. Commitment means a firm, patient‑centered promise to follow the prescribed plan, even when progress feels slow. Consistency refers to adhering to the prescribed frequency, intensity, and technique, allowing the body to adapt safely. Communication involves regular dialogue with the chiropractor, physical therapist, and coaching staff to report pain, fatigue, or psychological concerns, ensuring the program is adjusted promptly. Together, these pillars create a holistic, evidence‑based pathway to a safe return to sport and full activity.
Pain Peaks and Chiropractic Care Planning
Pain Peaks & Chiropractic Session Planning
| Tissue Type | Pain Peak Time Post‑Injury | Typical “Worst Day” | Chiropractic Session Recommendation |
|---|---|---|---|
| Muscle (highly vascular) | 48‑72 h | 2‑3 days | 4‑6 weekly visits for acute relief; 8‑12 total for full course |
| Tendon / Ligament (poorly vascular) | 3‑5 days | 3‑5 days | Similar 8‑12 week protocol; may need extended maintenance |
| Lower‑back pain (mixed) | 2‑4 days (inflammatory) | 3‑4 days | 8‑12 weekly sessions, reassess strength ≥80‑90 % of contralateral side |
 When is the worst day after an injury?
When is the worst day after an injury?
Pain typically peaks during the inflammatory phase of tissue healing. For highly vascularized structures such as muscle, the greatest discomfort occurs around 48–72 hours post‑injury, while tendons and ligaments—being poorer in blood supply—often reach their most painful point between days 3 and 5. This "worst day" window reflects the body’s protective response, limiting movement to safeguard the injured tissue.
How many chiropractic sessions are typically needed for lower‑back pain?
Evidence from clinical practice indicates that most patients begin to experience meaningful relief after 4–6 weekly chiropractic visits. A standard protocol usually comprises 8–12 appointments, spaced once per week, incorporating spinal adjustments, soft‑tissue work, and therapeutic exercises. The exact number varies with injury chronicity, overall health, and response to treatment; acute cases may resolve sooner, whereas chronic or complex presentations often require additional sessions or a maintenance phase. Ongoing reassessment ensures the plan is adjusted to achieve pain‑free range of motion, restored strength (≥80‑90 % of the contralateral side), and functional readiness for return to daily or sport‑specific activities.
Posture, Statistics, and Documentation
Posture, Statistics & Documentation
| Metric | Value / Statistic | Source / Note |
|---|---|---|
| Sessions needed for noticeable posture improvement | 6‑10 weekly sessions | Based on clinical observations |
| Patients reporting clear pain reduction after chiropractic care | 70‑80 % | Research meta‑analysis |
| Patients reporting functional gains (ROM, ADL) | ~60 % | Clinical outcome studies |
| Reduction/Elimination of prescription pain meds | 40‑50 % | Patient‑reported outcomes |
| Surgery avoidance after care | Up to 30 % | Comparative cohort data |
| Overall patient satisfaction | >90 % | Survey data |
| ACA Documentation Requirements | Subjective history, objective findings, treatment plan, informed consent, progress notes | American Chiropractic Association guideline |
 How many chiropractic sessions are needed to improve posture?
How many chiropractic sessions are needed to improve posture?
Improving posture generally requires a series of focused chiropractic treatments rather than a single visit. Most patients notice meaningful changes after 6 to 10 weekly sessions, which give the spine and supporting musculature time to adapt. The exact number varies with the severity of the postural deviation, any underlying conditions, and the patient’s adherence to a prescribed home‑exercise program. During each appointment the chiropractor evaluates alignment, performs adjustments, and teaches targeted stretches and strengthening drills that reinforce the correction. Consistent at‑home work often leads to lasting posture improvement within this timeframe.
What are the key statistics on the benefits of chiropractic care?
Current research shows that 70‑80 % of patients experience a clear reduction in pain after a course of chiropractic care. Approximately 60 % report measurable gains in functional ability and range of motion, enabling a quicker return to daily activities. Between 40‑50 % of patients reduce or eliminate reliance on prescription pain medication, including opioids, and up to 30 % avoid surgery altogether. Patient‑satisfaction surveys consistently exceed 90 % for overall experience and perceived health benefits.
What documentation guidelines does the American Chiropractic Association recommend?
The ACA advises a comprehensive record for each patient, beginning with a detailed subjective history (chief complaint, medical background, lifestyle factors). Objective findings—ROM measurements, orthopedic and neurological exam results, imaging—must be recorded precisely. A clear treatment plan outlining adjustments, modalities, education, and expected outcomes, plus a signed informed‑consent form, is required. Ongoing progress notes tracking symptom changes, functional status, and plan modifications ensure continuity of care and legal compliance.
Concussion Return‑to‑Play and Tissue Healing
Concussion RTP & Tissue Healing Timeline
| RTP Step | Activity | Minimum Duration | Advancement Criteria |
|---|---|---|---|
| 1. Symptom‑limited rest | Bed rest, no activity | 24 h | No symptoms for 24 h |
| 2. Light aerobic | Walking, stationary bike (no weight‑lifting) | 24 h | Symptom‑free for 24 h |
| 3. Moderate activity | Light jog, light resistance, head‑movement | 24 h | Symptom‑free for 24 h |
| 4. Heavy non‑contact drills | Sprinting, high‑intensity bike, sport‑specific drills | 24 h | Symptom‑free for 24 h |
| 5. Full‑contact practice | Controlled contact drills | 24 h | Symptom‑free for 24 h |
| 6. Competition | Full sport participation | — | All previous steps completed without symptom recurrence |
| Tissue Healing Phase | Approx. Days | Main Processes | Chiropractic Role |
|---|---|---|---|
| Inflammatory | 0‑3 days | Clot formation, debris clearance | Soft‑tissue work, inflammation control |
| Proliferative | 3‑21 days | Collagen synthesis, granulation, angiogenesis | Adjustments to promote proper alignment, controlled loading |
| Remodeling | >21 days (weeks‑months) | Collagen re‑orientation, scar maturation, tensile strength gain | Ongoing adjustments, therapeutic exercise, biomechanical optimization |
 The CDC’s 6‑step Return‑to‑Play (RTP) protocol for concussion begins with a minimum 24‑hour period of symptom‑limited rest once acute signs have cleared. Step 2 introduces light aerobic activity (e.g., walking, stationary biking) without weight‑lifting, requiring another symptom‑free day. Step 3 adds moderate activity that raises heart rate and incorporates body or head movement, such as moderate jogging and light resistance work. Step 4 progresses to heavy, non‑contact drills—including sprinting, high‑intensity biking, and sport‑specific maneuvers—while still avoiding head impact. After a symptom‑free day, Step 5 permits full‑contact practice under controlled conditions, and Step 6 allows competition once all previous steps have been completed without symptom recurrence. Each step must last at least 24 hours and be monitored by the athlete, parents, coaches, and a healthcare provider.
The CDC’s 6‑step Return‑to‑Play (RTP) protocol for concussion begins with a minimum 24‑hour period of symptom‑limited rest once acute signs have cleared. Step 2 introduces light aerobic activity (e.g., walking, stationary biking) without weight‑lifting, requiring another symptom‑free day. Step 3 adds moderate activity that raises heart rate and incorporates body or head movement, such as moderate jogging and light resistance work. Step 4 progresses to heavy, non‑contact drills—including sprinting, high‑intensity biking, and sport‑specific maneuvers—while still avoiding head impact. After a symptom‑free day, Step 5 permits full‑contact practice under controlled conditions, and Step 6 allows competition once all previous steps have been completed without symptom recurrence. Each step must last at least 24 hours and be monitored by the athlete, parents, coaches, and a healthcare provider.
Tissue healing follows three overlapping phases. The inflammatory phase (≈0‑3 days) stops bleeding, forms a clot, and initiates debris clearance. The proliferative phase (≈3‑21 days) builds new collagen, granulation tissue, and blood vessels, laying the foundation for strength. The remodeling phase begins around three weeks and may continue for months, during which collagen fibers realign, mature, and the tissue regains tensile capacity. Controlled loading and chiropractic adjustments during these phases can improve alignment, reduce scar formation, and support a safe, evidence‑based return to full activity.
Stress Management and Integrated Care
Stress Management & Integrated Care
| Stress Effect | Chiropractic Impact | Integrated Strategies |
|---|---|---|
| Elevated cortisol → impaired healing, poor sleep, higher pain perception | Adjustments improve autonomic balance, reduce sympathetic over‑activity | Mindfulness breathing, adequate protein, vitamin D, magnesium, omega‑3 supplementation |
| High‑altitude outdoor lifestyle (e.g., Glenwood Springs) | Supports active rehab while protecting tissues | Low‑impact cross‑training (cycling, swimming), nutrition counseling, stress‑reduction techniques |
| Rehabilitation progression | Pain‑free ROM → swelling control → strength (80‑90 % opposite limb) → functional tests (single‑leg hops) | 3‑out‑of‑10 pain rule, recovery log, gradual load increase |
 Chronic stress drives up cortisol, which can impair healing, disrupt sleep, and increase pain perception. Evidence suggests that spinal adjustments improve autonomic balance, reducing sympathetic over‑activity and allowing the parasympathetic system to lower cortisol levels. Patients who receive regular chiropractic care often report calmer moods, better sleep quality, and reduced anxiety, all of which support a healthier endocrine response and faster tissue repair.
Chronic stress drives up cortisol, which can impair healing, disrupt sleep, and increase pain perception. Evidence suggests that spinal adjustments improve autonomic balance, reducing sympathetic over‑activity and allowing the parasympathetic system to lower cortisol levels. Patients who receive regular chiropractic care often report calmer moods, better sleep quality, and reduced anxiety, all of which support a healthier endocrine response and faster tissue repair.
In Glenwood Springs the high‑altitude environment and active outdoor culture demand a holistic rehab approach that blends chiropractic adjustments with low‑impact cross‑training, nutrition counseling, and mindfulness techniques.
A typical program begins with pain‑free range‑of‑motion and swelling control, then progresses to strength (80‑90 % of the opposite limb) and functional tests such as single‑leg hops.
Throughout, clinicians monitor a recovery log, adjust load based on the 3‑out‑of‑10 pain rule, and incorporate low‑impact cardio (cycling, swimming) to maintain cardiovascular fitness while protecting healing tissues. By integrating stress‑management strategies—breathing exercises, adequate protein, vitamin D, magnesium, and omega‑3 intake—with biomechanical care, patients achieve both physiological and psychological readiness for a safe return to sport and daily activity.
Putting It All Together for a Safe Return
Successful return to activity hinges on meeting clear milestones: pain‑free walking ≥30 min, no swelling or instability, 80‑90 % strength and ROM symmetry, and passing functional tests (single‑leg balance, hop symmetry, squat depth). Your Glenwood chiropractor will design a personalized program that blends adjustments, soft‑tissue work, low‑impact cross‑training, nutrition guidance, and a structured run‑walk interval plan. Continue tracking symptoms, maintain strength and cardio sessions, and schedule periodic re‑evaluations to sustain long‑term health.
